All About Homebirth Care
The Butterfly Position - an extension of McRobert's maneuver
Recently, I was asked about a maneuver I use that I call the Butterfly position. It is a step beyond McRobert's when needing to create more room at the pelvic inlet and outlet at the symphysis pubis. I use this maneuver when a momma is in McRobert's but needs a bit more space, especially with a slow-coming head or the step right before moving her into the Gaskin maneuver or Runner's (Parker's) position with a shoulder dystocia.
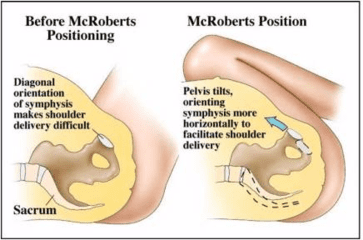
McRobert's is bending the knees and hyper-flexing the legs into the abdomen, bringing the knees straight up toward the ears. The position lifts the sacrum and tailbone off the bed, allowing the sacrum and tailbone the mobility to open up and create more space in the pelvis and shift the shoulder off the symphysis pubis.
The Butterfly position is a step beyond McRobert's. The legs are kept hyper-flexed, but the knees are moved away from the midline laterally to create greater space at the junction of the symphysis pubis. I would encourage you to experience this yourself. Lay on your back, put your fingers on top of your symphysis pubis, and then put your legs in the McRobert's position. Now, don't move your fingers and move your knees away from midline laterally, or butterfly them, keeping the ankles in line with the knees. You will feel the space at the symphysis pubis become wider due to the cartilage stretch.
The Butterfly position is very similar to the position which occurs when a momma holds her legs herself, grasping behind the knees during the 2nd stage. But with McRobert's, the care providers are pushing the legs back, and the momma's hands end up elsewhere. The Butterfly position is to push the legs back, like in McRobert's, and then to the sides, very much like a squat, but while reclining.
My mommas birth in a variety of positions, but when they are lying in their beds, and a bit more space is needed, especially when the birth of the head is slow, this is an option that often helps.
Marilee Pinkleton, CPM
Heartsong Midwifery, LLC
January 8, 2017
Copyright 2017-2022 Marilee Pinkleton
A New Perspective - Estimated Due Range (EDR)
“What’s Your Due Date (EDD)?” How about an EDR?
You are newly pregnant and meeting with your best friend for lunch to tell her of your good news. She excitedly says, “Congratulations!” and then asks, “What’s your due date?”
The date your friend is referring to, the Estimated Due Date or EDD, is a date typically given to a pregnant woman at her first prenatal visit. It is a calculated date created by taking the date of the first day of the last (normal) menstrual period (LMP), subtracting three months, then adding seven days. The result is a date that is approximately 280 days or 40 weeks from the LMP.
The EDD was created by German obstetrician, Franz Naegele (1778-1851), to describe the day at which half of all births occur earlier, and half of all births occur later. Only 5% of births occur on an EDD. Most births are clustered around the EDD; therefore, as many births occur after 40 weeks gestation as before 40 weeks.
What begins as a future day of great celebration often ends up as a date draped with anxiety, stress, and disappointment. Additionally, women are often faced with being defined as “early” when they have their babies before the EDD or “late” when they have their babies after their EDD, even if it is during term. Ask a pregnant woman, especially a first-time momma, and she will surely have the impression that the EDD, or very close to it, is supposed to be the birthday of her baby, or at least she hopes so.
A term pregnancy refers to the weeks during which a baby is considered to be developed to the point of being ready to be born. Term is 37–42 weeks of pregnancy, and term is considered to be normal. Although there are risks to consider on both sides of term, early and late, babies are still term from 37–42 weeks and are not post-dates until 42.1 weeks gestation.
If we know that 95% of the time, a woman will not have her baby on her EDD, what is a woman to do as she approaches her EDD, feeling the pressure of birthing on or very near that one day? What is she to do when her care provider begins talking about induction and interventions, based on the date of the EDD? How is she supposed to respond when family and friends call asking if she has had her baby yet?
I propose that we look at due dates in another way. For the women in my care, I use an EDR to denote the time frame during which the baby could be born. This stands for Estimated Due Range. I coined this phrase as it takes into account all the weeks of term: 37-42 weeks gestation. The 40-week date, as I call it, is, but 1 day out of 35 during which a woman can have her baby, or one day out of 5 weeks. If the EDR falls just right, a woman’s EDR could begin at the end of one month, run through the entirety of the next month, and into the beginning of the next month! The EDR will always include a date range including at least 2 months.
The following is an example of an EDR versus an EDD -- for an EDD of 2/20, the EDR is 1/23 – 3/6! When the EDR, 37 to 42 weeks gestation, falls across portions of 3 months, you can imagine the surprise on the woman’s face to know that her baby could be born in 1 of 3 months! I often see her shoulders and face soften. It seems like a very doable expectation to birth a baby during one of 35 days.
The EDR is a reflection of the term, which takes the focus off of the 1 (EDD) out of 35 days that she could, but probably won’t, have her baby. I believe this refocus is an important reframing.
Giving mother and baby the time they need to lead the journey of labor and birth most often gives the best opportunity for a healthy labor and birth. It also gives a woman the opportunity to come to the knowledge that her body works, and that she and her baby can do this amazing work.
How a woman feels about herself after birth is not the typical, measurable outcome of a maternity study, but it is important for the growth of a woman as a mother, partner, and person. She is not just her physical self, but a holistic being comprised of emotion and spirit as well. I had watched the confidence bloom in women when they realized they could do the work of labor and birth. As care providers, it is our job to pay attention to what we bring to the pregnant woman’s sacred space in how we care for and support her.
I believe if we can help reduce a woman’s stress by shifting the focus off of the one-day date of an EDD and onto the possibility of birthing sometime during the 35-day range of an EDR, we will make strides toward supporting the woman and her baby as best we can. Together the mother and baby will, almost always, begin their journey of labor and birth on just the right day for them.
Marilee Pinkleton, CPM
Heartsong Midwifery, LLC
Copyright 2013-2022 Marilee Pinkleton